Fungal InfectionsLast updated on Monday, April 20 2009 by gliageek
 
Aspergillus species grow on decaying vegetation and grain products, and are ubiquitous in the environment. Infection typically occurs in immunocompromised, usually neurtropenic, hosts. Aspergillus may also rarely produce brain abscesses and granulomas in individuals with a normal immune system. Abscesses are the result of hematogenous spread from pulmonary infection, contiguous spread from the sinuses, or direct inoculation due to trauma or surgery. CNS aspergillosis in the immunocompromised host usually presents with fever, confusion, and multifocal neurologic deficits. Common settings are neutropenia and organ transplantation. Aspergillus has a propensity to invade blood vessels, causing ischemic strokes and hemorrhages, as well as multiple abscesses. Pulmonary infiltrates are usually present, reflecting primary Aspergillus pulmonary infection. Diagnosis requires culture of pus from a brain abscess. Treatment involves draining of brain abscesses, and intravenous amphotericin B. 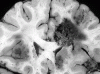  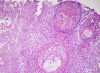 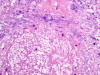
The rhinocerebral Syndrome is a progressive fungal infection of the sinuses, orbits, and brain usually caused by fungi of the order Zygomycetes. Infection begins in the sinuses, and is characterized by nasal congestion and discharge. Fungal hyphae then invade soft tissue and bone. There is often painless necrosis of the palate and nasal septum. Involvement of the orbit causes proptosis, ocular motility disturbance, and blindness. As with aspergillus, zygomycotic species are angioinvasive, often leading to thrombosis of the cavernous sinus and internal carotid artery. The syndrome is most common in diabetics (especially in ketoacidosis), neutropenic patients, organ transplant recipients, and those receiving chelation treatment for hemochromatosis (greater availability of iron speeds fungal growth). Imaging studies can confirm sinusitis, erosion of bone, and vascular involvement. Diagnosis is made by discovery fungal hyphae in necrotic tissue. Treatment involves debridement of infected tissue and intravenous amphotericin B.
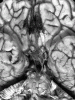 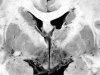
Aspergillus (and Mucorales) fungi are angioinvasive. Thus, like toxoplasma, they cause brain damage by occluding cerebral blood vessels. Unlike toxoplasma, however, these fungi cause vascular rupture, with hemorrhagic transformation of the coagulative parenchymal necrosis. While these organisms are large enough to be seen with routine stains, silver (GMS) or PAS stains highlight their morphology, aiding identification.
Related images: |
| Cerebral aspergillosis, coronal section, close-up.
Aspergillosis results in cerebral infarction with hemorrhagic transformation. |
|
| Cerebral aspergillosis, coronal section through the rostrum of the corpus callosum
Dissemination of the aspergillus organisms results in numerous hemorrhagic infarcts within the brain parenchyma. |
|
| Cerebral aspergillosis, brain biopsy, low power H&E.
Cerebral infection by Aspergillus results in coagulative necrosis, which is usually followed by hemorrhagic transformation |
|
| Cerebral aspergillosis, brain biopsy, high-power H&E.
On this high power photomicrographs of a blood vessel within the area of quite noted necrosis, filamentous organisms can be seen at the top third, representing infiltration of the vessel wall. |
|
| Neonatal cerebral candidiasis, whole mount
Innumerable microabscesses are typically seen in neonatal cerebral candidiasis. |
|
| Neonatal cerebral candidiasis, coronal section, close-up.
On gross examination, the candidal microabscesses are seen as pasty white circumscribed lesions clustering around the gray-white junction |
|
| Acute meningitis secondary to Coccidioides, cerebellum, low power H&E stain.
Even at this low power, fungal organisms can be identified within the inflammatory process |
|
| Cranial nerve inflammation secondary to coccidial meningitis, H&E stained section
Peripheral (cranial) nerve can be seen at the upper left hand corner of the photograph. At the lower right is be cerebellar molecular layer. |
|
| Coccidiodes meningitis, high-power H&E stain
Coccidiodes endospores, both within spherules and free within the meninges |
|
| Cryptococcoma, middle cerebellar peduncle, transverse section.
Cryptococcoal organisms are normally confined to the perivascular (Virchow-Robin) spaces. This patient's parenchymal involvement occurred secondary to damage incurred during stereotactic biopsy procedure |
|
| Cryptococcal meningitis, high-power H&E stained section.
Cryptococcal organisms can be seen as translucent soap bubble within the inflammatory exudate. |
|
| Cryptococcal meningitis, coronal section, close-up view of cerebral cortex and meninges.
Cryptococcal meningitis often causes marked thickening of the arachnoid space secondary to the high mucopolysaccharide content of the organisms wall. At the same time, paucity of acute inflammation results in very little brain swelling as seen here. |
|
| Histoplasmoma, H&E stained section, high-power.
Histoplasmosis may cause CNS disease in an immunocompromised and elderly patients. It is the smallest of the yeasts seen within brain infections, where it is typically seen within macrophages |
|
| Mucormycosis, secondary to Zygomycetes infection, coronal section through basal ganglia.
Rhinocerebral mucormycosis gives rise to bilateral hemorrhagic necrosis at the base of the brain overlying the cribriform plate. |
|
| Mucormycosis, secondary to Zygomycetes infection, ventral surface of brain.
Bilateral hemorrhagic necrosis of olfactory bulbs and adjacent cerebral cortex due to rhinocerebral mucormycosis |
|
| Phaeohyphomycosis, basal lateral surface of brain.
Phaeohyphomycosis results in multiple areas of hemorrhagic necrosis, identical to that seen with aspergillosis. |
|
| Phaeohyphomycosis, coronal section of brain, close-up.
Hemorrhagic necrosis, secondary to vascular damage by fungus. |
|
| Phaeohyphomycosis, lateral surface of brain.
Multiple areas of hemorrhagic necrosis can be seen on the surface of the brain due to this angiotrophic fungal infection. |
|
| Phaeomycosis, Gomori methenamine Silver staining x 600
Silver positive filamentous organisms resembling aspergillus. |
|
| Phaeomycosis, low power H&E stained section.
Necrosis with hemorrhagic transformation. |
|
| Phaeomycosis, high power H&E stained section
Phaeomycosis is caused by naturally pigmented fungi, unlike other fungal infections of the nervous system. |
|
| Phaeomycosis, PAS stained section x100
Filamentous organisms are present within this blood vessels wall |
|
| Candidial microabscess, PAS 600x
Both yeast and pseudohypha forms can be seen with PAS staining |
|
| Cryptococcoma, H&E stain section, high power
Acute, chronic, and granulomatous inflammation containing cryptococcal organisms. |
|
| Neonatal candidiasis, PAS stain x 200
Microabscesses containing numerous candidal organisms |
|
| Neonatal candidiasis, PAS stain whole mount section
Innumerable candidal microabscesses with predilection for grey-white junction |
|
| Cryptococcoma, mucicarmine staining, high power
Cryptococcus is unique among CNS infectious fungal organisms in that the mucopolysaccharide capsule stain strongly with mucicarmine histochemistry. |
Related review questions: |
| Infections 01
Which of the following fungal organisms is most likely to result in this gross appearance |
|
| Fungal CNS Infections 01
Which of the following fungi is commonly seen primarily in the Ohio and Mississippi basins |
|
| Fungal CNS Infections 02
A 35 year-old male billionaire playboy is brought into Gotham City emergency room by his butler and his young male live-in companion. The patient is stuporous and vomiting. The butler explains that the patient has had a several week history of slowly progressive... |
0 user entries
|
|