Vascular Disease 4: Other topics in vascular diseaseLast updated on Friday, April 17 2009 by gliageek
Working from the outside in, intracranial hemorrhage may be epidural, subdural, subarachnoid, intraparechymal, or intraventricular in origin (though many do not remain localized to a single compartment). The term “hemorrhagic stroke” only applies to subarachnoid and intraparenchymal hemorrhages. Epidural and subdural hematomas most often result from traumatic head injury. Intraventricular hemorrhage is an important affliction of premature infants. Intraparenchymal hemorrhages are most often associated with hypertension, but may also be due to vascular malformations (usually presenting in young patients) or amyloid angiopathy (nearly confined to elderly patients). The proximate pathogenesis of hypertensive brain hemorrhage is controversial. In the setting of chronic hypertension, an abrubt increase in blood pressure associated with an increase in cerebral blood flow is hypothesized to produce bleeding from normal or injured vessels. Active bleeding usually lasts less than an hour. Progressive clinical deterioration after bleeding has stopped is usually due to cerebral edema or systemic metabolic derangements, although prolonged bleeding may occasionally be responsible, especially with continued uncontrolled hypertension. While hypertensive hemorrhages may occur anywhere within the brain, they are most commonly seen in the same locations as lacunar infarcts, and for the same reason (small vessels arising directly from large caliber arteries).     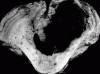
The most common cause of non-hypertensive intracerebral hemorrhage is cerebral amyloid angiopathy. In this disorder, the walls of leptomeningeal and intracortical arteries are infiltrated by a protein which is nearly identical to that found in senile plaques of Alzheimer’s disease. Necrosis of vascular smooth muscle ensues and the cerebrocortical arterioles become prone to rupture. This leads to the typical clinical picture of lobar hemorrhages (which are often multiple and recurrent) in an elderly patient.
    
Arteriovenous malformations (AVMs) are the most clinically significant of the congenital vascular malformations (the others are less likely to become symptomatic and are more frequently incidental findings on examination of the brain for other reasons). AVMs are congenital arterio-venous shunts or connections without intervening capillary beds. Two thirds are diagnosed before the age of forty. Ninety percent are in the cerebral hemispheres and most of these are in the middle cerebral artery distribution. AVMs tend to present either with intracerebral hemorrhages or seizures.
Subarachnoid hemorrhage may result from extension of an intracerebral hemorrhage. In the absence of intracerebral hemorrhage, subarachnoid hemorrhage occurs secondary to rupture of vessels within the subarachnoid space. Trauma is the most common cause of subarachnoid hemorrhage, however in trauma, subarachnoid hemorrhage is not a major contributor to overall morbidity and mortality.
The most important etiology of subarachnoid hemorrhage is rupture of a saccular aneurysm. Ruptured saccular aneurysms account for about half of all non-traumatic subarachnoid hemorrhages and produce death or permanent disability immediately in up to 50% of patients. In the absence of surgical intervention, many patients die from rebleeding if they survive the initial hemorrhage.
    
Saccular aneurysms are the most common form of intracranial aneurysm, and are found with a prevalence of 2-5% at autopsy. Predisposing factors include a family history of saccular aneurysm, polycystic kidney disease, coarctation of the aorta, and diseases that affect the integrity of vascular walls, such as Marfan’s syndrome, Ehlers-Danlos syndrome and pseudoxanthoma elasticum. Subarachnoid hemorrhage produces increased intracranial pressure, which can exceed the cerebral areterial perfusion pressure. This results from a variety of contributing factors including the volume of subarachnoid blood, vasogenic edema, blockage of CSF drainage, and impairment of cerebral venous drainage. 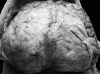
The exact cause of early mortality in SAH is often unclear but may be related to cardiorespiratory problems mediated by intense catecholeminergic output resulting from hypothalamic irritation. Cerebral vasospasm is the most important cause of morbidity and mortality in patients who survive the initial hemorrhage. This occurs in about 25% of patients, usually between 4 and 12 days after the initial hemorrhage. The clinical syndrome evolves over a period of hours or days, which differentiates it from rebleeding which is usually sudden. Although the pathogenesis of cerebral vasospasm after subarachnoid hemorrhage is far from completely understood, it seems to be related to the amount of blood surrounding the arteries at the base of the brain. It has been hypothesized that the release of oxyhemoglobin from lysing subarachnoid red blood cells initiates arterial smooth muscle contraction.
Further reading
Cordonnier C, Leys D. Stroke: the bare essentials. Pract Neurol. 2008 Aug;8(4):263-72. Related images: |
| Amyloid Angiopathy, H&E stain slide
Hyalin thickening of leptomeningeal blood vessels can be appreciated by H&E staining |
|
| Amyloid Angiopathy, immunohistochemical staining for beta amyloid
Except in rare familial transthyretin amyloidosis, amyloid angiopathy is always composed of beta amyloid, even in patients with non-beta amyloid systemic amyloidoses |
|
| Amyloid Angiopathy, immunohistochemical staining for beta amyloid, low power.
Immunohistochemical staining highlights beta amyloid deposition within the walls of leptomeningeal and intracortical blood vessels. |
|
| Lobar Hemorrhage, Coronal section through parietal lobes
Multiple, cortically based hemorrhages with extension into the white matter are characteristic of amyloid angiopathy related intraparenchymal hemorrhages. |
|
| Pineal Cyst demonstrating evidence of recent hemorrhage, close-up gross photograph
Hemorrhage originating within a glial cyst of the pineal region is rare, but may give rise to catastrophic subarachnoid hemorrhage (pineal apoplexy). |
|
| Intraparenchymal hemorrhage, horizontal section of brain
Hypertensive intracranial hemorrhage typically originates in the vascular distribution of penetrating arteries. In this patient, putaminal hemorrhage occurred secondary to rupture of lenticulostriate arteries penetrating from the proximal middle cerebral artery |
|
| Ceerebellar Hemorrhage, transverse section through the cerebellum and Pons
Ceerebellar Hemorrhage is considered a neurosurgical emergency for reasons which are apparent within this photograph. |
|
| Pontine Hemorrhage, sagittal section of brain
Pontine hemorrhage may occur secondary to hypertensive damage to penetrating pontine arteries originating from the basilar artery. |
|
| Pontine Hemorrhage, multiple transverse sections through brainstem and cerebellum
Hypertensive pontine hemorrhage in an anti-coagulated patient, with devastating consequences |
|
| Putaminal Hemorrhage, Coronal section through brain
Hypertensive damage to lenticulostriate arteries causing intraparenchymal hemorrhage with ventricular rupture and transtentorial herniation. |
|
| Thalamic Hemorrhage, Coronal section of brain
Hypertensive damage to the thalamoperforant arteries originating from the proximal trunks of the posterior cerebral artery, resulting in thalamic and intraventricular hemorrhage. |
|
| Intramedullary spinal cord hemorrhage, gross photograph of ventral surface of spinal cord
Although the majority of significant spinal cord hemorrhages occur consequent to traumatic injury, patients with severe coagulopathies, such as this leukemic patient, they also demonstrate intramedullary spinal cord hemorrhage |
|
| Intramedullary spinal cord hemorrhage, transverse section through thoracic spinal cord.
Intramedullary spinal cord hemorrhage in the absence of trauma may occur in patients with severe coagulopathies. |
|
| Superficial cerebral cortical hemorrhages, coronal section through parietal lobe.
Although usually encountered in elderly patients with amyloid angiopathy, superficial femoral cortical hemorrhages in younger patients may be secondary to mycotic aneurysm in the setting of bacteremia such as may occur in patients with subacute bacterial endocarditis. |
|
| Fusiformvertebro-basilar aneurysm, dissected circle of Willis.
Vertebrobasilar fusiform aneurysms are rare, but may be encountered in patients with fibromuscular dysplasia. |
|
| Superficial siderosis, ventral surface of brain.
Superficial siderosis is an unusual condition resulting from chronic blood leakage within the subarachnoid space. Breakdown products of heme accumulate in the dependentleptomeninges and are toxic to Purkinje cells resulting in an ataxic syndrome. |
|
| superficial Siderosis, H&E stained section of medulla x 40
Hemosiderin laden macrophages can be seen within the leptomeninges and dissecting along perivascular spaces into the brainstem parenchyma |
|
| Superficial cirrhosis, H&E stained slide x 400
This high powered view of medulla demonstrates hemosiderin laden macrophages and associated swollen axons which occurred secondary to disruption of axonal transport, probably induced by the toxic effects of iron. |
|
| Sneddon Syndrome, dorsal view of brain.
Sneddon Syndrome is a progressive noninflammatory thrombotic vasculopathy affecting small vessels within the brain and skin. |
|
| Sneddon Syndrome, lateral surface of brain, close-up
Sneddon Syndrome is a progressive noninflammatory thrombotic vasculopathy affecting small vessels within the brain and skin. This close up view of the surface of the cerebral cortex demonstrates numerous small pits, each representing infarcts related to occlusion... |
|
| Thrombotic thrombocytopenic purpura, horizontal section of brain through basal ganglia.
Patients with thrombotic thrombocytopenic purpura often demonstrate thromboses within distal small caliber vessels within the brain, leading to multiple microinfarcts and microhemorrhages often manifest as intractable epilepsy/status epilepticus. |
|
| Aneurysm wall, histochemical staining for elastin.
The normal vessel wall is present at the right side of the photograph. The aneurysm wall is characterized by absence of internal elastic lamina. |
|
| Aneurysm wall, high power H&E stain
Normal vessel wall at right gradually demonstrating architectural disorganization towards the left side of the photograph. |
|
| Aneurysm wall, H&E stained slide x 40
Normal blood vessel wall at lower right portion of photograph merging into aneurysm wall, which lacks internal elastic lamina and well-defined smooth muscle media. |
|
| Aneurysm wall, movat pentachrome stain x 40
Normal blood vessel wall at left side of photograph. Aneurysm wall at right, characterized by absence of internal elastic lamina and smooth muscle, with replacement by disorganized fibromyxoid tissue |
|
| Aneurysm wall, high-power movat pentachrome stain.
Normal vessel wall at left demonstrating termination of internal elastic lamina and well defined smooth muscle media at the base of the aneurysm wall at the center the photograph. |
|
| Aneurysm Wall, high power trichrome stain
Skeletal Muscle stains red with trichrome. Normal vessel wall at right demonstrating progressive thinning towards the aneurysm at the left of the photograph. |
|
| Diffuse cerebral edema, in situ photograph of dorsal surface of brain with dura
In this patient, diffuse cerebral edema occurred secondary to subarachnoid hemorrhage. |
|
| Giant saccular aneurysm, Circle of Willis, ventral surface of brain, close-up
This giant unruptured saccular aneurysm resulted in multiple cranial nerve deficits secondary to chronic compression. |
|
| Giant MCA aneurysm, ventral surface of brain.
Giant, thrombosed MCA aneurysm presenting as intracerebral mass lesion |
|
| Saccular aneurysm of posterior communicating artery, status post coil, ventral surface of brain, close-up
Note hemorrhagic swelling of adjacent to optic nerve. |
|
| Ruptured anterior communicating artery aneurysm status post clipping
Subarachnoid hemorrhage consequent to arterial rupture. |
|
| Ruptured MCA aneurysm, dissected
Rupture of this middle cerebral artery aneurysm resulted in fatal subarachnoid hemorrhage. |
|
| Ruptured saccular aneurysm, top of the basilar artery
Along with posterior and anterior communicating arteries and middle cerebral artery, the top of the basilar artery is a predilection site for cerebral aneurysms. |
|
| Subarachnoid Hemorrhage, ventral surface of brain
Rupture of saccular aneurysms involving the circle of Willis results in subarachnoid hemorrhage centered on the base of the brain. |
|
| Thrombosed Basilar artery aneurysm, transverse section through pons
This giant thrombosed basilar aneurysm resulted in cortical spinal tract impression bilaterally resulting in bilateral spasticity. |
|
| Amyloid Angiopathy, Congo red stain with polarization.
Amyloid can be defined by apple green birefringence upon polarization of Congo red stained sections. |
|
| Amyloid Angiopathy, Congo Red stained section
Amyloid demonstrates metachromasia of Congo red staining, resulting in a brick red appearance of amyloid deposits. |
|
| Amyloid angiopathy involving temporal artery, Congo red stained section with polarization
Congo Red stain of a temporal artery biopsy form a patient with amyloid angiopathy, viewed through a pair of polarizing filters. The bright green is the apple green birefringence that is characteristic of amyloid. |
|
| Temporal Artery, Congo Red stained section x 40
Metachromatic staining of amyloid deposits with brick red appearance |
|
| Amyloid angiopathy involving temporal artery, H&E stain x 20
Hyalin thickening of the arterial wall with loss of normal cellular components. Unlike leptomeningeal blood vessels where amyloid angiopathy is nearly always due to vascular involvement by beta amyloid, temporal arteries demonstrate vascular amyloid secondary... |
|
| Temporal Artery with Amyloid, H&E stain x40
Amyloid is characterized by extracellular amorphous appearing eosinophilic deposits which appear to compromise the integrity of the vascular wall through damage to normal medial smooth muscle elements. |
|
| CT SAH
This non-contrast head CT shows the presence of subarachnoid blood. |
Related pages:
0 user entries
|
|